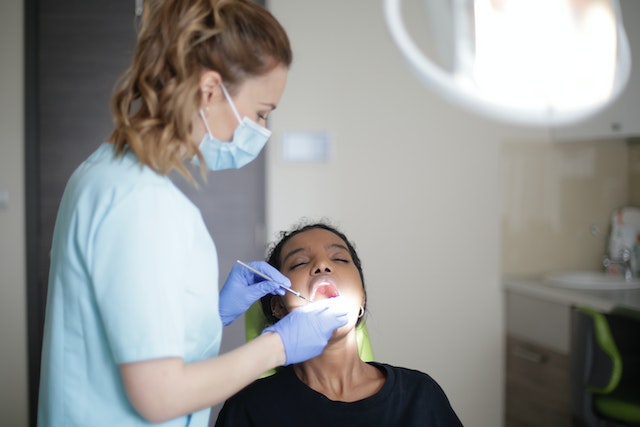
When you swallow, do you notice that it sometimes causes pain in the roof of your mouth? Likely, the majority of us don’t give the roof of our mouth as much consideration as other parts of our mouth, such as our teeth, tongue, or cheeks. If, on the other hand, anything is wrong with the roof of our mouth or if it aches, it is difficult, if not impossible, to ignore the problem. You will be aware of it whenever you speak, consume anything, or eat.
When swallowing causes the roof of the mouth hurts, the cause may be trauma (such as from biting down on something hard), burns (from eating something too hot), or even an oral infection of some kind. We are fortunate that, similar to the rest of our oral tissue, our palate may mend reasonably. When swallowing causes pain on the roof of the mouth for more than ten to fourteen days in a row, you should make an appointment with your dentist for an examination and an oral cancer screening for a professional assessment.
What leads to the painful and swollen condition of the roof of the mouth? Inflammatory conditions are almost always the source of pain felt on the roof of the mouth hurts. Inflammation may be caused by systemic disorders or environmental factors that irritate the mucosal lining of the mouth, which can lead to the development of sores. The following information may assist you in better understanding your symptoms and determining whether or not you need to see a medical professional.
Reasons for inflammation
Because it plays a role in the body’s defence against various infectious agents and poisonous chemicals, the mouth is particularly prone to inflammation by various infectious agents and other factors.
Infectious: painful sores may form in the mouth, particularly on the soft or hard palate, as a symptom of bacterial infections, which their presence may identify. Fungi are another kind of microorganism that may infect parts of the body that are warm and humid, such as the mouth. Fungi may cause painful areas ranging from red and spotty to creamy and white in appearance.
Pain in the roof of the mouth brought on by an allergy may be a sign of a potentially fatal drug response, requiring prompt medical treatment. Various medications, including those meant to treat infections, epilepsy, and even mood disorders, have been shown to cause severe skin and mucosal responses in some patients.
Inflammation of the gums, also known as gingivitis, may be caused by a lack of proper dental care and a buildup of germs.
Autoimmune: Systemic autoimmune disorders that affect numerous body parts, such as inflammatory bowel disease and lupus, often appear with symptoms that affect the mouth. Autoimmune rheumatoid arthritis is another example of an autoimmune ailment that affects the mouth.
Acute necrotizing ulcerative gingivitis, often known as ANUG, is an infection of the gums that occurs only in very severe cases. It is also known as “trench mouth” because it was seen in many troops entrapped in trenches during World War I.
Medical causes
Pain in the gums, swelling of the gums, and brown, blue, or black discoloration of the skin within the mouth are all symptoms of mucosal melanoma, a rare form of cancer.
Burning mouth syndrome, often known as BMS, is a chronic pain syndrome that manifests as a burning sensation in the mouth. Nobody knows what caused it.
Environmental causes
It is common for food and liquids to enter the mouth first. You may feel discomfort or an allergic response that will have a more severe impact on the roof of your mouth hurts.
Irritants: Both alcohol and tobacco are known to be among the most irritating substances to the human body. They are known to irritate the mouth to a substantial degree and have even been linked to the development of some cancers. Both tobacco and alcohol may increase the number of cells that develop in the mucosal lining of the mouth as a consequence of persistent irritation and dehydration, which can cause excruciating sores to form in that area.
The most prevalent factor in the development of mouth ulcers is a traumatic experience. Trauma may be caused by a direct injury, such as a blow or a fall to the face or mouth; however, trauma can also be caused by indirect injuries, such as loose fillings, ill-fitting dentures, and even braces.
Viral throat infection
Similar viruses to those that cause the flu and the common cold also often produce a sore throat. When infected individual coughs or sneezes, the virus is released into the air and may be caught by someone else who breathes it in or contacts an infected surface.
Genital herpes
This virus causes herpes simplex virus type 1 infection. Transmission occurs by kissing or other oral intercourse with a person who has active sores. People usually have a cluster of mouth sores and other symptoms, including fever, headache, sore throat, and swollen lymph nodes during the initial outbreak. This is usually the most painful stage.
Cancer of the oral cavity
Only around 10% of all melanomas begin in the head and neck, and only about 1% of all malignant melanomas are mucosal melanoma of the head and neck (MMHN). It has a dismal prognosis and is more prevalent among the elderly.
Influenza, or the common cold
Common cold symptoms include a hacking cough, stuffy or runny nose, red eyes, and a sore throat. It’s not uncommon for children to have more than eight colds a year, and most people get at least two or three.
Get some shut-eye and a hefty dose of H2O. If you or someone you’re around has a cold, avoiding personal contacts with them, such as a hug, kiss, or handshake, is best. Most cases of the common cold clear up within 7-10 days.
Herpes Simplex Virus
Herpes simplex viruses 1 and 2 are responsible for cold sores. When no apparent sore is present, the sores may spread via close, personal contact like kissing or oral sex.
It is more common among sexually active young people, although anybody may get it. Towels, dishes, and other shared items may include all harbor the infection.
The lips, nose, and cheeks may feel tingly or burn for up to a day before the blisters form. Fever, sore throat, and other flu-like symptoms are also possible.
Though there is currently no treatment for herpes simplex, cold sores may be treated to reduce pain and the risk of spreading the infection.
Typically, the blisters clear up in about a month, but the virus might reactivate at any moment since it has not been eliminated from the body. Some people find that taking antiviral medication or using an antiviral cream helps speed up recovery.
Urea-rich necrosis
Canker sores are tiny, grayish-white lesions that may appear anywhere in the mouth but most often on the tongue, lips, and inside of the cheeks. Canker sores have an unknown etiology. However, they seem to be genetically predisposed to allergies and nutritional deficiencies.
Chlorhexidine mouthwashes (Peridex or Periogard) or steroid medicines may be used to treat this problem without a doctor’s supervision (Orabase, Betnesol, or Ovar).
Syndrome of the Burning Mouth
Without an identifiable trigger, continuous burning pain or feeling in the mouth is known as burning mouth syndrome (BMS), a chronic pain condition. Women are 7 times more likely to experience this than males, which usually occurs during hormonal transitions (just before or during menopause). The origin is unknown. However, it may be related to saliva composition, denture wear, tics such as teeth grinding, infections, or autoimmune disorders.
In the next weeks, you should see your primary care physician. In such a setting, the doctor will do diagnostic tests to rule out other potential sources of your discomfort. There are treatments available if the burning mouth condition is the root cause. Unfortunately, therapy is not always effective.
Conclusion
Pain and discomfort on the roof of your mouth may have several different origins, ranging from health issues like oral cancer to imbalances in nutrition and electrolytes, as well as oral trauma or injury. Depending on the underlying reason, discomfort and pain may be accompanied by various additional symptoms, some of which may need prompt or emergency medical attention.